Congratulations to Whitaker Wander 5k runners and walkers!
Over 100 people participated in the Whitaker Wander 5k, the most since the event's beginning, and almost $8000 was raised towards the Health Center's programs and services.
Read more
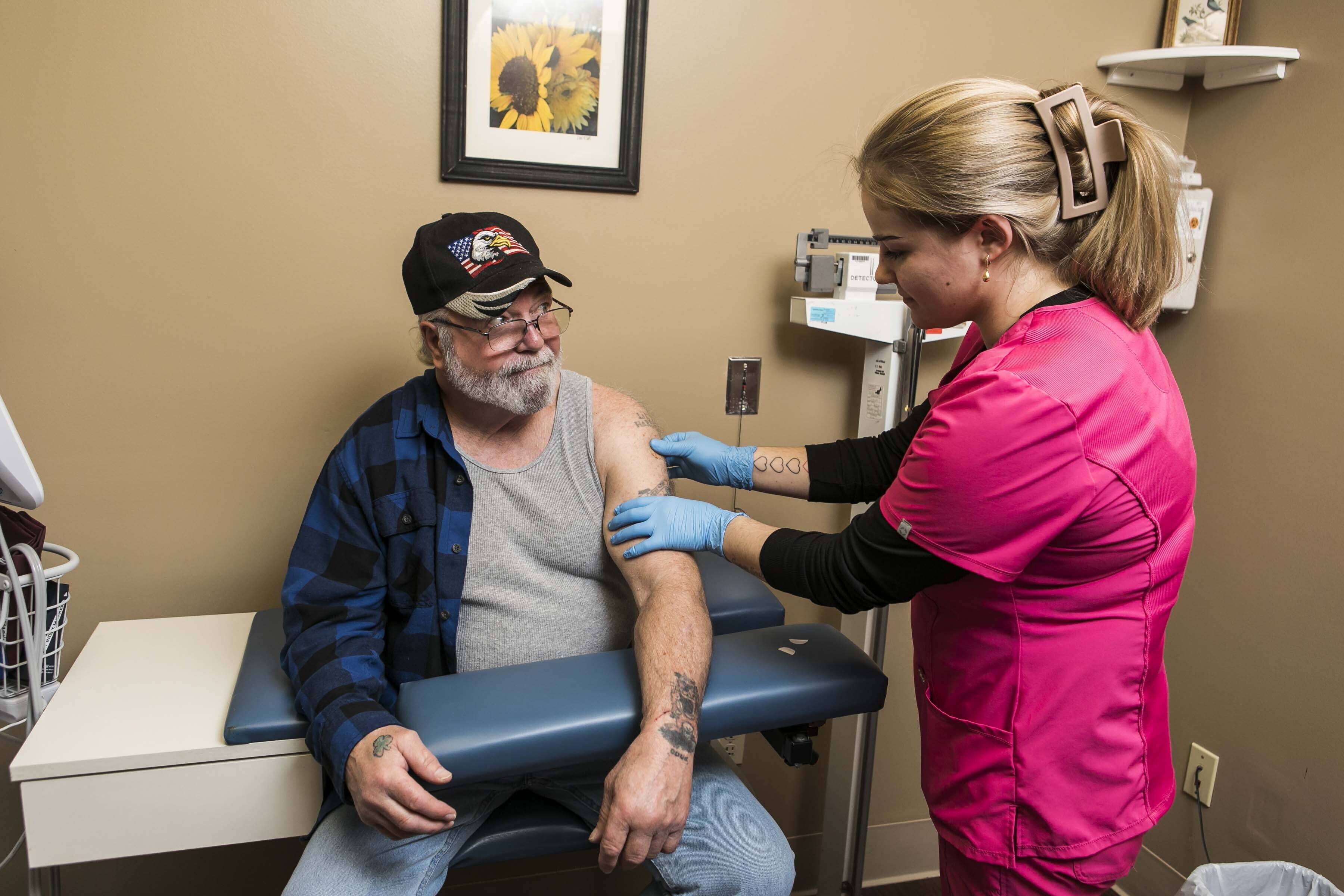
At the heart of White Mountain Community Health Center is an innate goal to care for the whole person. With empathy and understanding, we work with our patients to meet them where they are and develop care plans that are uniquely personal. The health center is for anyone seeking approachable care to take ownership of their health and live well, regardless of health status or income.
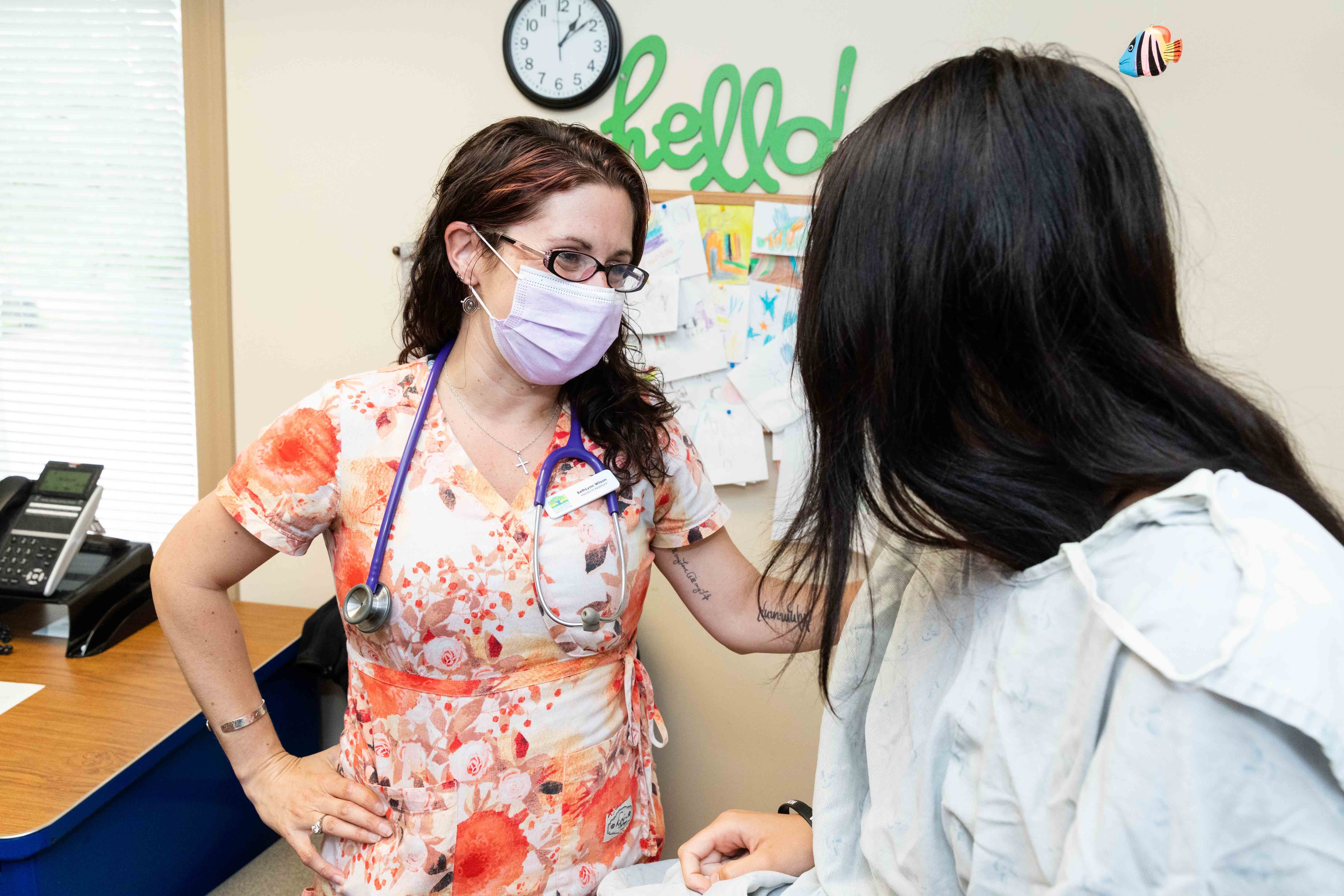




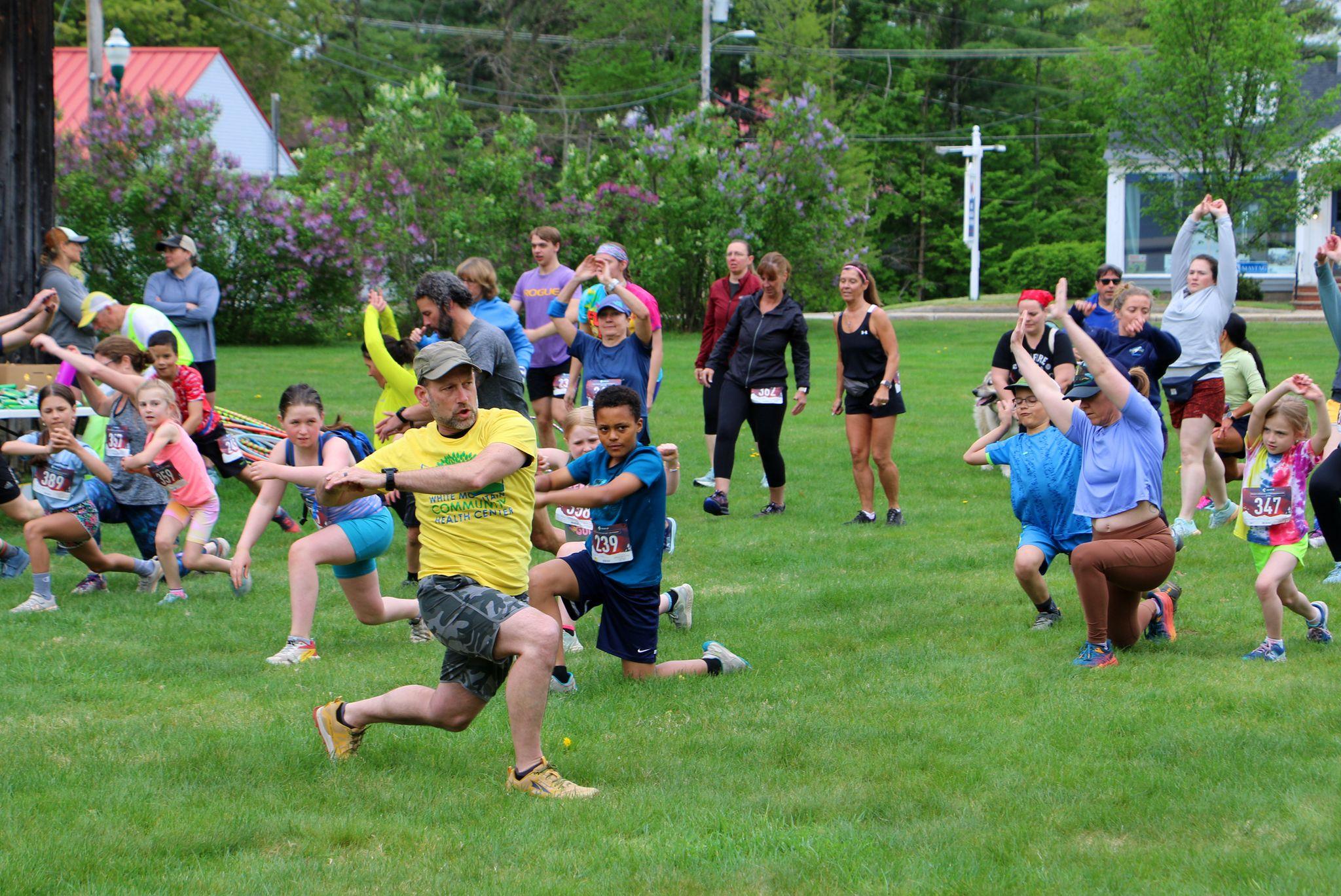
First time patients can find out what to expect from a visit and how to prepare before coming in here.
Donations and support from our community help make it possible for us to treat anyone, no matter what's going on in their lives.